Abstract
Purpose
To present a classification system for vertebral body osteonecrosis (VBON) based on imaging findings and sagittal alignment and consequently to propose treatment guidelines.
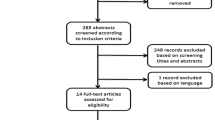
Methods
Chart review and classification of imaging and clinical findings. An analysis of literature about VBON has been evaluated to conceive the classification. The current data allows to correlate radiological findings with different stages of the pathophysiological process and consequently to propose a patient-tailored treatment plan.
Results
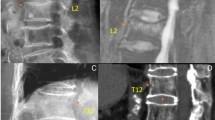
The classification identifies 4 stages: stage 0 (theoretical phase), stage 1 (early phase), stage 2 (instability phase) and stage 3 (fixed deformity phase). Local (angular kyphosis expressed as anterior–posterior wall height ratio) and global (sagittal vertical axis and pelvic tilt) sagittal alignment are considered as complementary modifiers to tailor the most suitable treatment. Stage 1 is generally managed conservatively. Stage 2 and 3 often require different surgical approaches according to local and global sagittal alignment.
Conclusions
The classification allows a systematic staging of this disease and can help establish a proper and patient-oriented treatment plan. Further researches are advocated to fully validate the proposed classification system.
Graphical abstract
These slides can be retrieved under Electronic Supplementary Material.





Similar content being viewed by others
References
Shah KN, Racine J, Jones LC, Aaron RK (2015) Pathophysiology and risk factors for osteonecrosis. Curr Rev Musculoskelet Med 8(3):201–209
Lafforgue P (2006) Pathophysiology and natural history of avascular necrosis of bone. Jt Bone Spine 73(5):500–507
Ma R, Chow R, Shen FH (2010) Kummell’s disease: delayed post-traumatic osteonecrosis of the vertebral body. Eur Spine J 19(7):1065–1070
Young WF, Brown D, Kendler A et al (2002) Delayed post-traumatic osteonecrosis of a vertebral body (Kümmell’s disease). Acta Orthop Belg 68:13–19
Swartz K, Fee D (2008) Kummell’s disease: a case report and literature review. Spine (PhilaPa 1976) 33(5):E152–E155
Hajnovic L, Sefranek V, Schütz L (2017) Influence of blood supply on fracture healing of vertebral bodies. Eur J Orthop Surg Traumatol. https://doi.org/10.1007/s00590-017-2069-7. [Epub ahead of print]
Fabbriciani G, Pirro M, Floridi P et al (2012) Osteoanabolic therapy: a non-surgical option of treatment for Kümmell’s disease? Rheumatol Int 32:13714
Rossini M, Viapiana O, Gatti D et al (2010) Capacitively coupled electric field for pain relief in patients with vertebral fractures and chronic pain. Clin Orthop Relat Res 468(3):735–740
Heo DH, Choi JH, Kim MK et al (2012) Therapeutic efficacy of vertebroplasty in osteoporotic vertebral compression fractures with avascular osteonecrosis: a minimum 2-year follow-up study. Spine (Phila Pa 1976) 37(7):E423–E429
Vanni D, Pantalone A, Magliani V et al (2017) Corpectomy and expandable cage replacement versus third generation percutaneous augmentation system in case of vertebra plana: rationale and recommendations. J Spine Surg 3(3):379–386
Zhang GQ, Gao YZ, Chen SL et al (2015) Comparison of percutaneous vertebroplasty and percutaneous kyphoplasty for the management of Kümmell’s disease: a retrospective study. Indian J Orthop 49(6):577–582
Formica M, Basso M, Cavagnaro L et al (2016) Kümmell disease: illustrative case for definition criteria. Spine J 16(10):e707–e708
Cho Y (2017) Corpectomy and circumferential fusion for advanced thoracolumbar Kümmell’s disease. Musculoskelet Surg 101(3):269–274
Zhang X, Hu W, Yu J, Wang Z, Wang Y (2016) An effective treatment option for Kümmell’s disease with neurological deficits: modified transpedicular subtraction and disc osteotomy combined with long-segment fixation. Spine (Phila Pa 1976) 41(15):E923–E930
Lim J, Choi SW, Youm JY et al (2017) Posttraumatic delayed vertebral collapse: Kummell’s disease. J Korean Neurosurg Soc 61(1):1–9
Nakamae T, Fujimoto Y, Yamada K et al (2017) Relationship between clinical symptoms of osteoporotic vertebral fracture with intravertebral cleft and radiographic findings. J Orthop Sci 22(2):201–206
Libicher M, Appelt A, Berger I et al (2007) The intravertebral vacuum phenomenon as specific sign of osteonecrosis in vertebral compression fractures: results from a radiological and histological study. Eur Radiol 17:2248–2252
Yu CW, Hsu CY, Shih TT et al (2007) Vertebral: MR imaging findings and related changes on adjacent levels. AJNR Am J Neuroradiol 28:42–47
Nardi A, Tarantino U, Ventura L et al (2011) Domino Effect: mechanic factors role. Clin Cases Miner Bone Metab 8(2):38–42
Garbossa D, Pejrona M, Damilano M et al (2014) Pelvic parameters and global spine balance for spine degenerative disease: the importance of containing for the well being of content. Eur Spine J 23(Suppl 6):616–627
Diamond TH, Clark WA, Kumar SV (2007) Histomorphometric analysis of fracture healing cascade in acute osteoporotic vertebral body fractures. Bone 40(3):775–780
Piazzolla A, Solarino G, Lamartina C et al (2015) Vertebral bone marrow edema (VBME) in conservatively treated acute vertebral compression fractures (VCFs): evolution and clinical correlations. Spine (Phila Pa 1976) 40(14):E842–E848
Formica M, Cavagnaro L, Basso M, Zanirato A, Felli L, Formica C, Di Martino A (2016) Which patients risk segmental kyphosis after short segment thoracolumbar fracture fixation with intermediate screws? Injury 47(suppl 4):S29–S34. https://doi.org/10.1016/j.injury.2016.07.048
Zanirato A, Damilano M, Formica M et al Eur Spine J (2018). https://doi.org/10.1007/s00586-018-5535-y. [Epub ahead of print]
Krüger A, Oberkircher L, Figiel J et al (2015) Height restoration of osteoporotic vertebral compression fractures using different intravertebral reduction devices: a cadaveric study. Spine J 15(5):1092–1098
Funding
There is no funding source for this article.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
Pedro Berjano received honorarium for surgeons’ education activities from Nuvasive, Medacta, DepuySynthes and his department received unrestricted research grants from Nuvasive, Medacta, DepuySynthes and K2 M. Claudio Lamartina received honorarium for surgeons’ education activities from Nuvasive, Medacta, DepuySynthes and K2 M and his department received unrestricted research grants from Nuvasive, Medacta, DepuySynthes and K2 M. No other disclosures by the rest of authors.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Formica, M., Zanirato, A., Cavagnaro, L. et al. Vertebral body osteonecrosis: proposal of a treatment-oriented classification system. Eur Spine J 27 (Suppl 2), 190–197 (2018). https://doi.org/10.1007/s00586-018-5600-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00586-018-5600-6